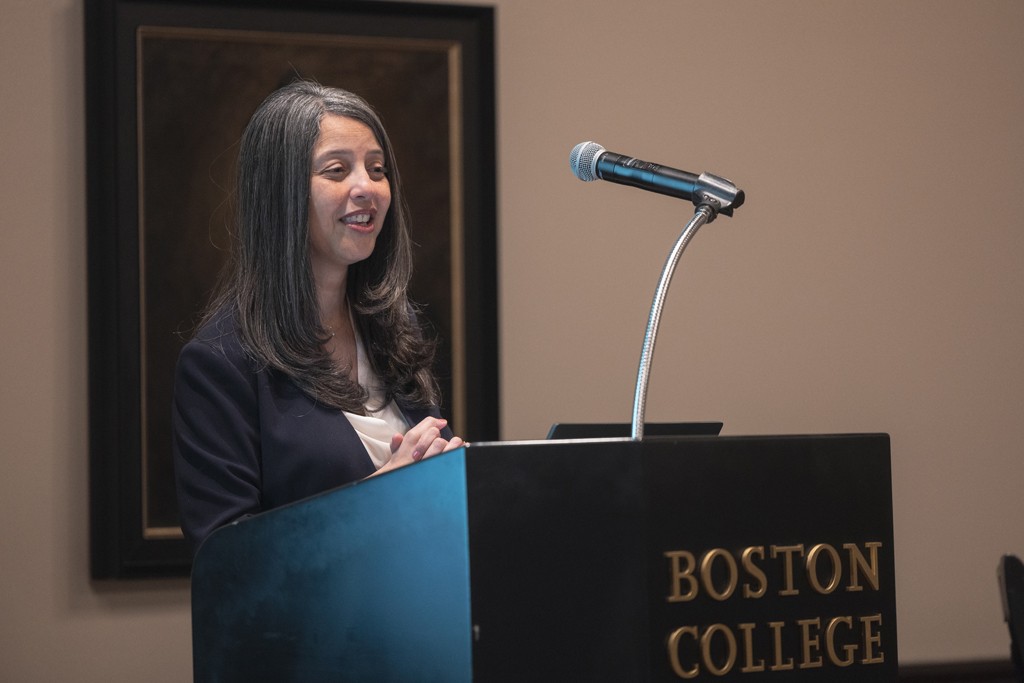
Elsie Taveras delivers the keynote address at the 2023 Equity, Justice, and Inclusion Lecture and Distinguished Alumni Awards Celebration. Photo by Chris Soldt.
Boston is one of the healthiest cities in the United States, according to Elsie Taveras, the inaugural chief community health and health equity officer for Mass General Brigham. But the city is home to stark and persistent racial disparities in chronic health conditions and mortality rates, Taveras said at Boston College on February 6, and the COVID-19 pandemic has exacerbated these inequities.
Black residents of Suffolk County, which comprises the cities of Boston, Chelsea, Revere, and Winthrop, had higher COVID mortality rates than their white counterparts, according to stats cited by Taveras. And Black mortality rates from non-COVID causes spiked in 2020, the height of the pandemic. But white mortality rates from non-COVID causes decreased over the same time period.
“What COVID revealed were stark inequities and vulnerabilities in minority communities—as well as historic underinvestment in community health and structural racism that has led to tremendous disparities in health outcomes for some populations in Boston,” said Taveras, who gave the keynote address at Boston College School of Social Work’s annual Equity, Justice, and Inclusion Lecture and Distinguished Alumni Awards Celebration.
Her lecture—delivered to a live audience in 100 Gasson Hall and to a virtual audience on Zoom—focused on MGB’s multi-million-dollar initiative to combat the impact that racism has had on patients, staff, and the wider community. The largest health system in Massachusetts launched “United Against Racism” in 2020 in response to civil unrest and protests against racist violence, aiming to eliminate disparities in patient care, create workforce equity, and improve community health.
“We had to take a deep look at how we as a health system were contributing to some of these inequities,” said Taveras, “and start to think of what could we be doing differently to do our part in changing what has been an historic difference in health outcomes in the city of Boston.”

Associate Professor Summer Hawkins, left, nominated Sarah B. Coughlin for the Distinguished Alumni Award. Photo by Chris Soldt.
After MGB launched the initiative, Taveras and her colleagues surveyed more than 1 million patients to better understand the population that they serve. They asked questions that zeroed in on their patients’ race, ethnicity, language, gender identity, and need for accommodations.
One of their biggest findings was that many patients lacked access to both the internet and software platforms used in digital care. So MGB provided patients with iPads, gave them access to the internet, and hired digital access coordinators to link patients with online services.
“If we don’t know enough about our patients, then we can’t create incredible programs that will lead to improving access for those patients,” said Taveras, who also works as a pediatrician at Mass General Hospital.
The initiative’s work is focused on 21 clinics in MGB’s health system that serve a high percentage of patients who identify as Black, Indigenous, or People of Color, Taveras said. 59,000 patients at these clinics have hypertension, according to a PowerPoint slide she showed during her talk, including 15,000 Black and Hispanic patients with high blood pressure.
Over the past 18 months, every patient at these clinics has completed an assessment of their social risk factors, which have been shown to play a major role in health. Patients with high blood pressure who have at least one social risk factor—perhaps they lack housing or have trouble paying for medicine—have been matched with community health workers and behavioral health clinicians to help improve their physical and mental well-being. The early results have been good: Since February 2022, the percentage of Black and Hispanic patients who have their blood pressure under control has increased 3 percent.

Salem Professor in Global Practice Theresa Betancourt, left, nominated Ngozi Enelamah for the Distinguished Recent Alumni Award. Photo by Chris Soldt.
“We’re making the case that it’s not just important to treat hypertension with a statin, but that it’s just as important to treat hypertension with behavioral and mental health support and social risk mitigation,” said Taveras. “Some of the early findings of our model show that it works. That if you can support patients not just with the clinical services that they need, but help them mitigate their social risk factors, we’re able to show a return on investment on hypertension and blood pressure control.”
She said the United Against Racism initiative is also working to address a profound mental health crisis, noting that rates of anxiety, depression, and substance use have spiked since COVID hit in the spring of 2020.
As part of a $25 million investment in community health initiatives and programs, MGB formed a partnership with BCSSW in 2021 to improve the mental health of Latinx communities in Massachusetts. Last November, the health system gave the Latinx Leadership Initiative a $600,000 grant to develop the workforce of bilingual and bicultural social workers in the state. Four LLI students have already completed the program, which provides stipends and professional development to fellows as they work in community health settings that predominantly serve Latinx clients, and, going forward, the LLI and MGB will select at least 10 fellows each academic year.
“Not only do we have a mental health and behavioral health crisis, but we have a workforce crisis. We don’t have enough BIPOC social workers working hand in hand with our clinicians to tackle the crisis we are seeing,” said Taveras. “MGB invested in community partners and educational institutions like BC to grow the behavioral health workforce across the Commonwealth and we couldn’t be happier with some of the work that’s happening across the 20-plus organizations we have funded. Some of this work has gone to support a very diverse workforce, including the LLI, which is developing social work leaders equipped to work with Black and Latinx communities.”
In a Q&A following her talk, Taveras expanded on MGB’s partnership with the LLI, a cohort-based program that prepares bilingual and bicultural social workers to accompany Latinx communities in developing sustainable solutions to complex problems in health, education, housing, and other areas. She praised LLI Founding Director Rocío Calvo for working to embed students in community health clinics where clients might typically have limited access to social workers who speak their language.
“We need more of these programs that introduce our workforce to the settings where we are seeing the greatest health inequities,” she told Assistant Professor María Fernanda Piñeros-Leaño, who moderated the discussion. “I’m incredibly proud of the work happening here at the School of Social Work. I’m incredibly proud to be part of these partnerships and investments across the state to do our part in tackling that workforce crisis.”
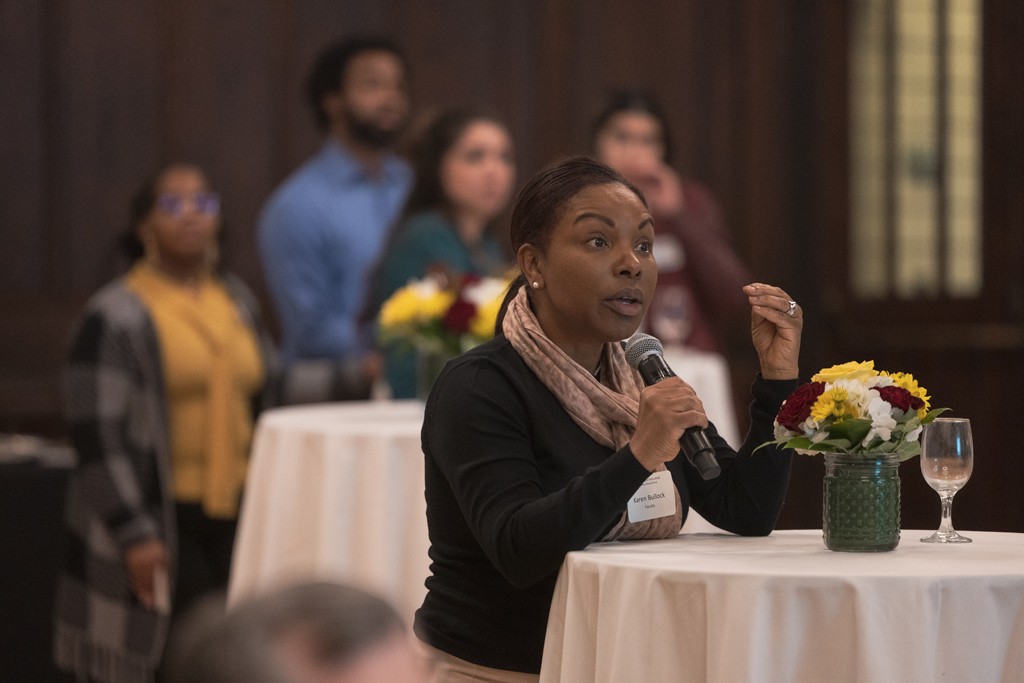
Karen Bullock, the Louise McMahon Ahearn Endowed Professor at BCSSW, asks Taveras a question during the event. Photo by Chris Soldt.
As part of a video capping the event, alumni and community partners praised the LLI, which will celebrate its 10-year anniversary at the end of this academic year.
Dewin Hernandez, who graduated from the MSW/MBA dual degree program in 2021, acknowledged the LLI’s transformational impact on the social work field. “For everything you have done, are doing, and will do, you have my deepest gratitude,” he said. “I can not wait to see what the next 10 years will hold.”
A representative from Casa Esperanza, a bilingual and bicultural behavioral health clinic that specializes in serving the Latinx community in Massachusetts, said it has been a privilege to work with students, faculty, and staff in the LLI. “This unique program that is provided in the classrooms has made a tremendous difference in the work that we see with our population here at Casa Esperanza,” she said. “Thank you for paving the way. We’re looking forward to many more years of collaboration with the LLI.”
After Taveras’ talk, BCSSW honored two alumni for their impressive contributions to the field of social work. The School celebrates two graduates at the event every year, bestowing one award upon an alum who earned an MSW or PhD 10 or more years ago and another award upon an alum who earned an advanced degree between five and 10 years ago.

From left to right: Rocío Calvo, Elsie Taveras, María Fernanda Piñeros-Leaño, and BCSSW Dean Gautam N. Yadama. Photo by Chris Soldt.
Sarah B. Coughlin, MSW '07, who runs a private practice and works for the Center for Community Health Improvement at Massachusetts General Hospital, received the Distinguished Alumni Award. She said that Solution-Focused Therapy, taught by Associate Professor Susan Tohn, helped to shape her philosophy as a social worker.
“I don’t even think I knew at the time how influential this class would be as I started out my career,” said Coughlin. “She really challenged the notion that we needed as clinicians to focus on the problem of our clients, to focus on their trauma, to focus on their pain. She helped me understand the power of focusing on and tapping into human strength, the innate ability of clients to understand their own solutions, and the recognition that clients have all of the resources within themselves to heal, and that’s been the foundation of my clinical practice.”
Ngozi Enelamah, MSW '18, PhD '20, an assistant professor in the Department of Social Work at the University of New Hampshire, received the Distinguished Recent Alumni Award. Enelamah, whose research focuses on designing interventions to address mental health disparities in mothers and children in sub-Saharan African, Black U.S.-born, immigrant, and refugee families, shared two lessons that she learned from her time at BC: Work hard and go to events—you never know who you’ll meet, what you’ll learn, or how your newfound knowledge could shape your career path.
“One lesson was showing up to events such as this, where you meet one person or hear an idea that will help chart the course for your next move,” she said. “The other is hard work. The rigor of a program where you’re put to work—that stays with you, and I’ve carried that with me in my work.”


