When an 11-year-old girl appears in an emergency room with a broken foot, treating nurses and doctors routinely ask the obvious: How did this happen? But rarely do they follow up with questions that might lead to the discovery she is being bullied.

Judith A. Vessey
That could change as a result of a study led by Connell School of Nursing Professor Judith A. Vessey, a leading youth bullying expert and senior scientist at Boston Children’s Hospital. She is developing a screening tool to be called CABS—the Child-Adolescent Bullying Screen—a concise list of questions to be asked in clinical settings to detect adolescent bullying.
“If you don’t ask the next question, ‘Why were you running?’ you won’t learn she really was running away from friends, or that other kids stole or were playing keep-away with her possessions,” says Vessey, who holds the Leila Holden Carroll Chair in Nursing at the Connell School.
STEMMING THE TIDE
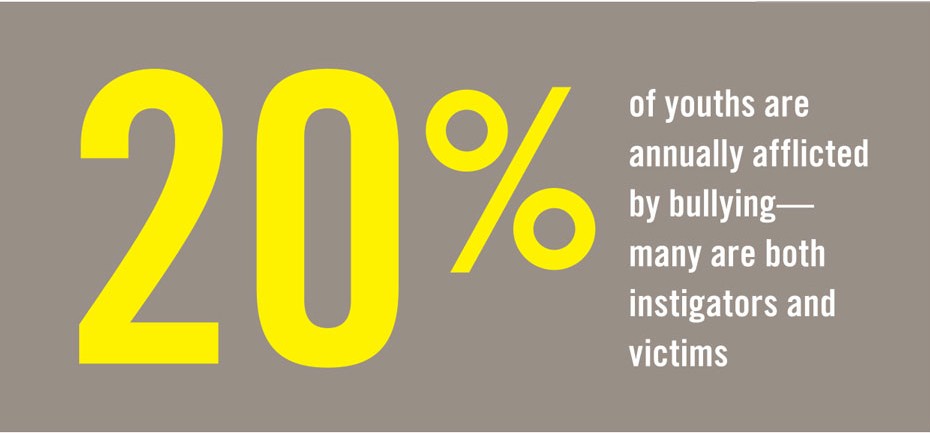
The rising tide of youth bullying is linked to an increasing toll of suicides, homicides, and other youth violence, and is recognized as a critical public health problem. Bullying annually afflicts at least 20 percent of youths—with many as both instigator and victim—according to multiple studies cited by Vessey and her co-investigators Rachel DiFazio, M.S. ’96, Ph.D. ’13, a pediatric nurse practitioner and nurse scientist at Boston Children’s Hospital, and Tania Strout, Ph.D. ’11, director of research for Maine Medical Center’s department of emergency medicine. In two-thirds of school shootings, longstanding bullying was a major motivation for the attack, according to studies Vessey cited in a review of bullying scholarship published in Nursing Outlook in 2013.
Much research has blamed bullying for higher rates of a host of short- and long-term health maladies, both medical and psychosomatic, Vessey says, including anxiety and depression, headaches, stomach aches, and upper respiratory problems as well as obesity and substance abuse.
“We know bullying victims have an increase in physical health problems from the chronic stress that suppresses the immune system, that’s why it’s something we need to focus on in the primary care arena,” says Vessey. The ill effects of bullying afflict instigators and recipients alike, and they also manifest in a full range of psychological challenges and academic performance issues that can last well into adulthood, Vessey and fellow researchers have found. It is no surprise, then, that reducing youth bullying is a major objective of state and federal legislation, and that in 2012, HealthyPeople 2020, a major US Department of Health and Human Services initiative, set a goal to reduce it by 10 percent.
BULLYING DEFINED
Not every mean remark or act is bullying, Vessey points out. According to seminal research by Norwegian expert Dan Olweus (which she cited in Nursing Outlook), scientists generally agree that bullying is characterized by three factors: a persistent pattern of verbal, nonverbal, or cyber-aggression that one or more youths inflict on another; deliberate intent to inflict physical, verbal, or emotional harm; and a real or perceived difference in power between instigators and recipients. Traditional, in-person confrontation and indirect bullying (spreading rumors, for example) have been augmented and amplified by cyber-bullying, where the power differential is increased exponentially by exposure on social media. Bystanders, Vessey has noted, play a significant role, providing the audience that ensures shame of the victim.
Passive recipients of bullying behavior “become more submissive, insecure, live in fear, restrict their activities, and do not readily defend themselves when they feel threatened,” Vessey’s research shows. But sorting out bullying situations can be complicated, she says. Bullying increases in middle school, when 32 percent of students experience it on a weekly basis—in part because that’s when students start to move from one classroom to another to change classes, increasing opportunities for anyone who is different to be bullied, Vessey observed in a 2014 article, “Measuring the Bullying Experience,” that appeared in the Journal of School Health. What’s more, she observes, “There’s a huge group of kids who are bullies and victims— a number of the kids who are bullies have parents who are bullies.”
TRADITIONAL FOCUS ON SCHOOL SETTINGS
In the past decade, 49 states have instituted anti-bullying laws, according to Vessey. Research on the problem has grown substantially, as has the number of anti-bullying programs in schools. But as Vessey sees it, there is little improvement to show for all the effort.
The focus of state and local government efforts has been to define and outlaw behavior associated with bullying, mandate anti-bullying school programs, and create specific criminal statutes with punishment ranging from school suspension to jail time. The drawback, Vessey says, is that most school programs are group oriented and designed to encourage empathy; they have had little effect on the prevalence of bullying, which produces high rates of absenteeism and diminished academic performance.
Even the most effective anti-bullying school programs don’t offer practical solutions. “You can build awareness but you don’t necessarily teach kids strategy: what to do when bullying is happening in front of their face.” Even when students can turn to a school nurse (or a school psychiatrist in some wealthier schools and systems), Vessey says, “Kids don’t feel there is privacy.” They fear that word will get around or they will be seen reporting to school administrators.
But while schools and legislatures have actively targeted the problem, organized health care, particularly nursing, has done little, according to Vessey. Indeed, while exploring the topic for Nursing Outlook, Vessey says she found scant attention paid to bullying in pediatric nursing. Her 2013 study pointed to a critical need for health care providers to take as active and systematic a role in screening for youth bullying as they do for other health concerns. Stepped-up efforts by health care providers are essential to identifying high-risk youths, detecting victims earlier, and curbing bullying’s cascading ill effects.
“Addressing bullying within a health context across health care settings is a nursing imperative,” Vessey’s article concluded.
DETECTION THROUGH PRIMARY CARD PROVIDERS
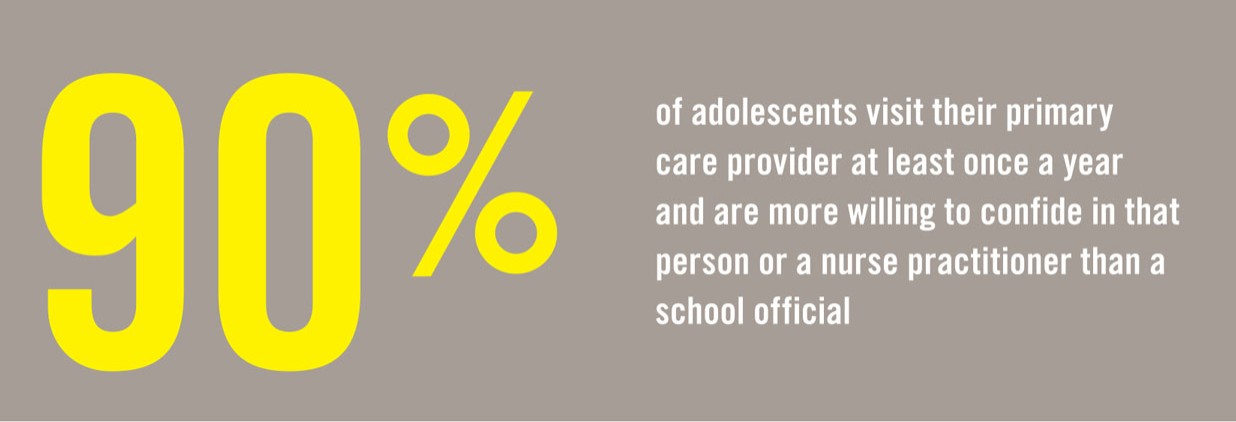
The fact that 90 percent of adolescents visit their primary care provider at least once a year recommends the clinical setting as the best venue to administer screening questions about bullying, Vessey says. “Adolescents are more willing to confide in their primary care provider or nurse practitioner,” she adds. Some primary care providers say they are already screening for bullying by simply asking, “Are you being bullied?” But Vessey says that the nature of bullying leads young patients to give overly subjective answers, under- or overreporting incidents.
Hence the need for a screening tool aimed at finding the kids who most likely are being bullied and most likely to suffer consequences, so health care providers can flag the right patients and refer them for fuller assessment.
Good tools exist for detecting signs of domestic violence and alcoholism, and the success of those instruments fuels hope for greater bullying detection. However, Vessey is mindful that screening for these and other public health imperatives—from prevalence of sexual activity to tobacco, alcohol, and drug use to depression to immunizations—is crowding the very brief time allotted to most routine clinical visits.
“The volume has just increased exponentially, and the time for the visits has been cut shorter and shorter,” Vessey says. “To tell any provider that you have to screen for one more thing is enough to make you go cross-eyed.” Any screening tool devised to detect bullying must be developed with that reality in mind. “If we want uptake by primary care providers it needs to be done in such a way that it is reliable, simple to administer, free, doesn’t take much time, and is acceptable to providers, parents, and kids,” she says.
Vessey wants to be sure that the CABS screen will be effective across cultural and socioeconomic groups. That’s why the study includes a range of adolescent participants from diverse cultural and socioeconomic backgrounds. Data is being collected throughout the Boston metropolitan area, Portland, and rural Maine.
IMPROVING INTERVENTION AND PREVENTION
Vessey is principal investigator of the CABS scale, which is funded by the Eunice Kennedy Shriver National Institute of Child Health and Human Development. The three-part mixed methodological study focuses on groups of young participants, asking what it means to be bullied and how they would feel if their primary care provider questioned them about it. The most illuminating responses will be vetted by an interdisciplinary group of clinical experts, principals, and counselors, then analyzed and winnowed further. The remaining questions will be put to 300 to 400 youths in a written questionnaire. Those results will be further analyzed and boiled down to four questions that can be quickly and easily incorporated in a doctor or nurse practitioner visit.
The goal of the screening questions is to identify youths involved in bullying earlier—even before the physical signs are clear—and intervene with medical and mental health treatment to curb harmful effects. Vessey’s aim is to reach victims as early as possible, at the annual trip to the doctor or in an emergency room visit, possibly sparing millions of adolescents further suffering.
“I want to focus on the middle group that is probably being bullied at school some, but hasn’t shared it with anyone yet.” Missing an opportunity to help them means a critical lag in identifying and intervening before negative effects develop. Vessey says, “We know that the earlier you come upon a problem, the easier it is to have success.”

—Judy Rakowsky, photograph by Lee Pellegrini, artwork by Christine Hunt