When Susan Wilkinson, M.S. ’14, worked as an emergency nurse for five years before graduate school, she often was struck by seeing people stigmatize those with mental illnesses. She developed a desire to work in mental health at the Connell School of Nursing (CSON) with its Jesuit traditions and championing of social justice. Now she has embraced it as a passion in the Mental Health Nurse Practitioner Residency program, a pioneering three-year partnership between the Connell School and the VA Boston Healthcare System that provides specialized training and professional development to nurse practitioners who work with veterans and their families.
Offering nurse practitioners the sort of extremely focused, on-the-job transitional training once reserved for physicians, the Mental Health Nurse Practitioner Residency pilot expands and strengthens the already strong bond that the Connell School and the VA Boston have developed while collaborating on a range of clinical training programs through the years.

Meeting the psychiatric and psychological needs of veterans is a pressing concern for the VA, and the Connell School’s strong curriculum in mental health helped the VA Boston land the mental health nursing residency, said Cecilia McVey ’72, the associate director of Nursing and Patient Services for the VA Boston Healthcare System. “If it were not for that base, I don’t think it would have been accredited,” she said. “But the program was funded to be one of the first in the United States.” (CSON is one of four similar mental health nurse residency partnerships nationwide. The others are the Birmingham VA Medical Center–University of Alabama at Birmingham, Durham VA Medical Center–Duke University, and the Ralph H. Johnson VA Medical Center–Medical University of South Carolina.)

TRAILBLAZING PARTNERSHIPS
CSON is also one of six Boston-area nursing schools that eight years ago formed the Northeast Region VA Nursing Alliance (NERVANA), which linked Boston, Regis, and Simmons colleges, Northeastern, the University of Massachusetts Boston, and UMass–Lowell with the VA Boston Healthcare System and the Edith Nourse Rogers Memorial Veterans Hospital in Bedford, Mass. The goal was to establish venues in which nursing students could provide care for veterans while improving their clinical skills, and supervising faculty augmented the teaching staffs at VA facilities as the VA enhanced its appeal as a future employer. The alliance has also provided a forum for clinical and academic partners concerned with patient care.
Experimental at first, NERVANA has been recognized as a national model: In October, the American Association of the Colleges of Nursing gave NERVANA its Exemplary Academic Practice Partnership Award.
“The best thing is to have that fertile exchange of the latest things in practice and the latest in academe,” said McVey, who was a driving force in establishing the regional alliance.

NERVANA’s initial focus was on hands-on undergraduate education at Boston and Bedford VA facilities. In 2012, the alliance added a postbaccalaureate 12-month nurse residency, in which RNs less than a year out of school acquire clinical experience to improve their skills and readiness for a career. (Each resident also develops an evidence-based research project during the year.) The residency, which grew to a class of 10 this year, has earned a three-year accreditation from the Commission on Collegiate Nurse Education. Two of the three CSON graduates who have participated in that program, Tiara Alston ’12 and Allison Cotta ’13, now work for the VA. Megan Hopper ’14 is a resident at the VA Boston’s AG unit in West Roxbury.
A DEDICATED UNIT FOR UNDERGRADUATE TRAINING OPENS
CSON’s newest foray with the VA is the January 2015 opening of a dedicated education unit (DEU) on the cardiothoracic surgical floor of the West Roxbury campus of the VA Boston. Clinical Associate Professor Stacey Barone oversees the Connell School unit, where she supervises and teaches six third-year CSON students in her Adult Health II Clinical course along with three staff nurses—postbaccalaureate resident alumna Alston is one—each of whom is paired with two CSON undergraduates.
The VA staff nurses supervise and train students like Anne O’Malley ’16, who welcomes the DEU experience. “For eight hours a week, I am taken through a typical shift and able to understand the critical thinking that is done with each nursing intervention,” O’Malley said. “Being part of the DEU has given me the opportunity to perform most daily tasks on my own with the guidance and support of my nurse.”
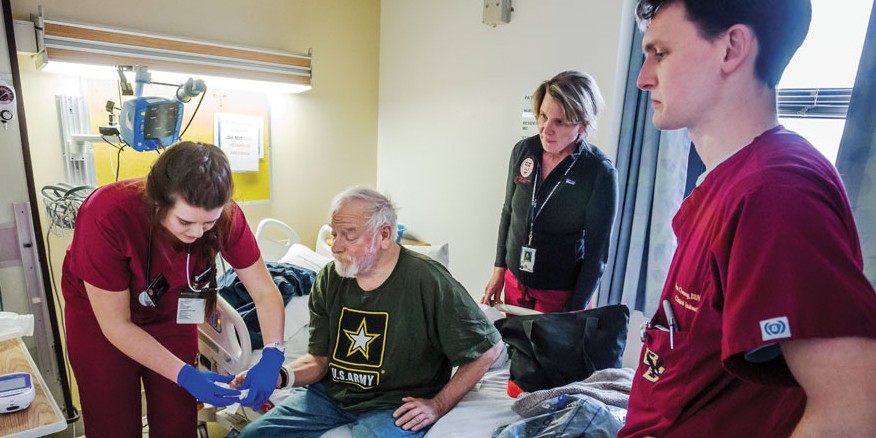
“This is a great opportunity for our students to get a fantastic learning experience from the staff, who teach them and empower them to become better nursing students,” said Barone. “And it’s a big cost to the hospital. They are paying the salaries of three nurses to be with the students.”
Because it is dedicated to training and supervising students, the VA experience offers them opportunities they might not have in other clinical settings, said Barone, who supervised clinicals for 12 years in the oncology unit at the Beth Israel Deaconess Medical Center. Research shows that a DEU offers better instruction and feedback from staff nurses about the latest equipment, medications, and practices.
“The best thing is to have [a] fertile exchange of the latest things in practice and the latest in academe.”
—Cecilia McVey ’72, Associate Director of Nursing and Patient Services, VA Boston Healthcare System
IMMERSION FOR NURSE PRACTITIONERS
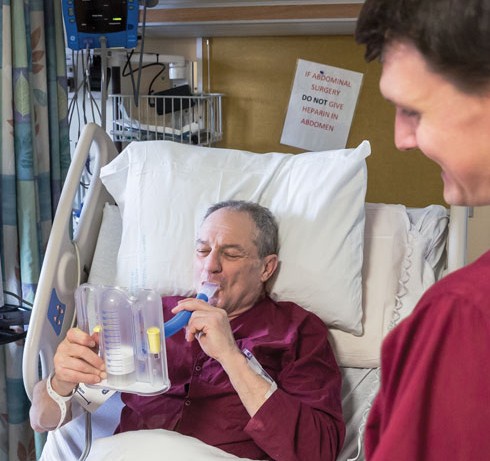
The 12-month Mental Health Nurse Practitioner Residency pilot program launched last summer, with Wilkinson and the other nurse practitioner residents in the VA Boston taking classes with Harvard Medical School psychiatry residents and rotating on multidisciplinary teams. “It’s very intense,” said Wilkinson, who was born in Uganda and competed nationally for one of four positions in the Boston program. “It helps you bridge the transition from the sheltered academic environment to the clinical.”
Rotations include acute inpatient, acute psychiatry, detox and residential treatment as well as triaging in an emergency room setting, said Sherley Belizaire, the VA’s director of the Mental Health Nurse Practitioner Residency. In addition, each resident works with a fixed group of counseling patients for the entire residency. They participate on teams that include an attending psychiatrist, a social worker, a psychologist, and other nurses, and interact with fellows in pharmacology and sociology, Belizaire said. They also learn about the latest research and most promising new therapies.

The clinical experience is invaluable, said Clinical Assistant Professor Pam Terreri, one of two CSON faculty advisors. “Most nursing graduates go through their academic training and emerge having met all the requirements for certification to operate in an independent role but they don’t have a lot of clinical experience to draw on,” she said.
The VA hopes the residency will become an enduring national model, a goal that Terreri and CSON Clinical Instructor Lori Solon are working on as they compare notes in regular conference calls with their peers in the other three-year pilots.
Admission to the program was extremely competitive, Belizaire said, with all applicants required to be 2014 nursing school graduates who completed board certification in time for the start of the program in July. And she said the Boston VA’s hope is for the program to grow beyond four slots and to be marketed nationally.
The Mental Health Nurse Practitioner Residency is filling a particularly strong need, said the faculty advisors. Nurse practitioners work more autonomously than other nurses and in many states they operate completely independent of physicians as they prescribe medications, and order lab tests, MRIs and CT scans.
Solon said the residency is critical to building confidence and skills while residents benefit from feedback and guidance. The VA is also an ideal teaching environment for nurse practitioners who focus on the patient in context. For instance, when an addiction outpatient has already gone through withdrawal and has left a structured setting, it is the nurse practitioner that helps figure out how well the veteran’s network of support is working and whether he has developed resources to stay sober. “They think about the whole patient,” said Solon.
Wilkinson said it is challenging to treat patients with many-layered diagnoses and fraught life situations: for example, veterans who are homeless as they struggle with posttraumatic stress or substance abuse problems.
“It’s a very tough population, there’s a lot going on,” said Wilkinson. “No matter how many appointments you secure, often they won’t show.”
The complexity of the cases the VA handles offers important experience as well as insight to residents, Solon said. No matter where they go on to work, they will be able to draw on knowledge of how best to treat veterans, whether or not their diagnoses are linked to exposure to trauma, and in some cases sexual trauma, she points out.
As challenging as Wilkinson finds the patients and the residency itself, “it’s really worth it,” she says. Wilkinson has developed a particular interest in addiction and substance abuse and in linking that work with psychiatry and medicine. And she wants to stay with the VA. “This is a really unparalleled opportunity. You are partnering with people who have been in the field so long and you get to learn from people who know so much.”
The partnership has been a great success from the VA’s perspective because it is attracting and retaining top-notch nurses while providing cutting-edge clinical experiences and developing best practices for treating veterans, McVey said. “Having all of those students exposed to the VA and my staff exposed to teaching in varying ways is just amazing; it’s helped the schools and us. I think it’s making better nurses to care for American veterans—and they are not just in veterans hospitals.”
—Judy Rakowsky, photographs by Caitlin Cunningham and Lee Pellegrini