(Photo: © Dorothy www.wearedorothy.com)
In 1948, 20 people in Donora, Pennsylvania, died from a toxic smog that enveloped the mill town for five long days. Twenty-one years later, Cleveland’s Cuyahoga River, glutted with factory waste, burst into flame—and not for the first time, either. That was how it used to be in the United States: the city air was thick and acrid, asbestos lined our buildings, Lake Erie was a “cesspool,” according to Time magazine, and so was Boston’s Charles River whenever a hard rain flushed it full of raw sewage.
But that was then. Today, we have all the benefits of the Clean Air Act, the Clean Water Act, and regulations that manage toxic chemicals. Our tap water runs clear, the air is fresh, and you can swim in the Charles River again. The world’s problems are myriad, but pollution is no longer among them—right?
Think again. In 2015, pollution and the diseases it can cause—including various cancers, stroke, heart and lung disease, neurodegeneration in adults, poor cognitive function, attention disorders, and autism-like symptoms in children—are estimated to have cost the world about $4.6 trillion and killed 9 million people. That is 16 percent of all the deaths worldwide. It’s three times more than die each year from AIDS, malaria, and tuberculosis combined, and more than are killed in all our many wars. And the news just gets worse: Fatalities related to outdoor air pollution—7 million a year—are on track to double in thirty years. Far from a problem of the past, pollution is deadlier than ever.
In the field of public health, Landrigan is a legend. He's overseen some of the most influential research of the past four decades, testified before Congress numerous times, and met with leaders from across the world.
Now, Boston College is launching a massive new effort to change the course of this deadly trajectory, and in so doing, to establish itself as a leader in global public health. Last summer, the university hired Philip Landrigan, Class of 1963 and one of the world’s most acclaimed environmental pediatricians and epidemiologists, to launch the new Global Public Health and the Common Good Program, as well as the first-of-its-kind Global Observatory on Pollution and Health. Together, the initiatives are charged with identifying and solving some of the world’s most pressing problems. With those goals, Landrigan is setting out to recruit and train a new generation of public health researchers ready to pick up the fight in a war to save lives that he has waged for the past 47 years.
* * *
You may not have heard the name, but there’s a good chance that Phil Landrigan has improved the health and safety of the people you love. In the public health field, he’s something of a legend. He’s the person who helped to get the lead out of our gasoline and paint, convinced the government to create new laws and agencies that protect children from pesticides and dangerous chemicals, and led the effort to document the devastating health effects suffered by workers and first responders in the aftermath of the 9/11 attacks. He has overseen some of the most influential public health research of the past four decades, testified before Congress numerous times, and forged relationships with leaders from across the world—crucial skills for the head of a new public health program launched with the ambitious goal of working with governments and international organizations such as the World Health Organization and the United Nations to address the major public health challenges of our time.
“He’s been an extraordinarily productive and important person in public health and global health,” said Jeffrey Koplan, the onetime director of the U.S. Centers for Disease Control and Prevention (CDC) who is now vice president for global health at Emory University. “I think the world of him.”
Maida Galvez, the director of the New York State Children’s Environmental Health Center, put it more succinctly. Landrigan, she told me, is considered “the father of the field of environmental pediatrics. He’s awesome—literally awesome.”
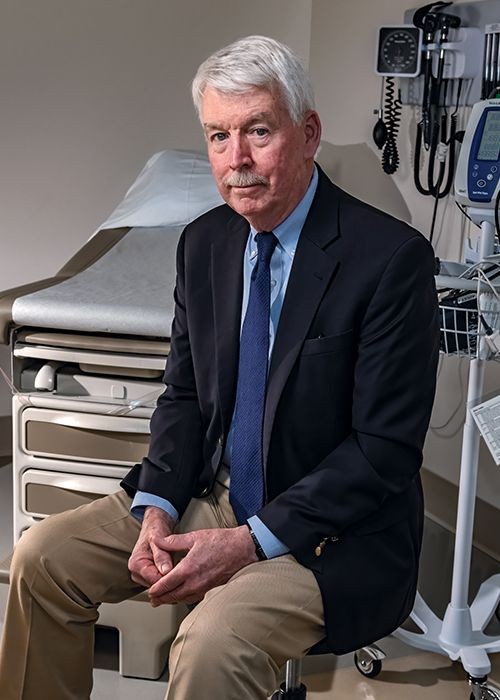
Dr. Philip Landrigan ’63, photographed in May in Maloney Hall. (Photo: Gary Wayne Gilbert)
Now Landrigan has taken on his next great challenge. Building a public health program is no easy task, and in the year since he officially rejoined his alma mater, Landrigan has been a whirl of activity. He’s launched a half-dozen projects that span the globe; secured a grant from the prince of Monaco’s foundation to combat the epidemic of plastics and other contaminants accumulating in our oceans; co-led a student service mission to Honduras; met with various heads of state and ministers of health; and, with university officials, signed a memorandum of understanding with the United Nations Environment Programme. “It’s like a revolving door,” said Tom Chiles, vice provost for research and academic planning and the DeLuca Professor of Biology. “Everybody knows him. It’s amazing.”
One day in April, in between Landrigan’s travels, meetings, and classes, I managed to catch up with him in his offices on the sixth floor of Higgins Hall. For the headquarters of a university’s massive new public health push, the room was relatively simple: a broad desk lined with tidy stacks of paper, a whiteboard on the wall listing various research projects currently under way—CVD, Monaco, India, Wellcome. (“We’re still in limbo on that last one,” he told me. “It’s in peer review.”)
Landrigan is tall and lean, with white hair and a matching mustache that he has worn for 25 years. At 76, he remains a vigorous presence. (He used to run marathons, and still goes to the gym.) As we talked in his office, Landrigan said the opportunity to launch a new public health program appealed to him for a number of reasons, but really, it came down to the fact that failing to address the looming pollution crisis “will make it impossible for modern society to survive.” It’s all laid out in a report that he and some colleagues recently published, he told me. “In the very first line of the introduction, we used the phrase ‘existential threat,’” he said. “Modern society depends on reasonably clean air and water. It needs sea levels that don’t rise. If all those things abruptly change, then the complex societies we’ve built in the last millennia will have real difficulty surviving in their present form.”
* * *
Landrigan grew up in the West Roxbury neighborhood of Boston. His parents were both schoolteachers, but inspired by his uncle, an ophthalmologist, he settled on medicine. He followed his father and uncles to Boston College. After graduating in 1963, he attended Harvard Medical School, and then spent a year stitching up knifing and gunshot injuries at Cleveland Metropolitan General Hospital.
Returning from Ohio, Landrigan served for two years as a pediatric resident at Boston Children’s Hospital. He finished his training in 1970, a time when, in accordance with the Vietnam War’s doctor draft, many young male physicians in the country were required to perform two years of national service. Landrigan wound up becoming an officer in the CDC’s elite Epidemic Intelligence Service. Most of the CDC’s focus back then was on communicable diseases—measles, rubella, rabies—but a call came in one day that was instead related to environmental public health. Landrigan’s life would never be the same.
On the other end of the phone line, a health officer in El Paso, Texas, shared his suspicions that a local ore smelter was dumping lead into the environment around the city. Landrigan and a colleague traveled to El Paso and, after conducting a series of tests, confirmed that the smelter was indeed contaminating the city’s air, soil, and dust—and was responsible for the shockingly high levels of lead in the blood of area children.

In the 1970s, Landrigan found that pollution from the Asarco smelting plant in El Paso, Texas, was responsible for elevated levels of lead in the blood of area children. The company eventually paid the government $1.79 billion to clean up sites in some 20 states. (Photo: University of Texas at El Paso Library, Special Collections Department)
Landrigan wanted to run another study, to see just what this lead might be doing to the children. He expected the city’s leaders to embrace the project. Instead, he told me, the members of the board of health made it clear that he wasn’t welcome in El Paso. “There was nothing subtle about it,” he said. So he marched into the state attorney general’s office and announced that he and his team were being impeded in their attempt to protect the children of El Paso. The AG assured him that the situation would be addressed. Landrigan was just 29 at the time. “Back then,” he told me, “we were cowboys.”
In El Paso, Landrigan and his team went on to produce some of the very first research establishing that chronic exposure to lead in the environment can cause a devastating reduction in IQ and neurologic function in children. That research, along with work by Herbert Needleman, then at Harvard, helped to persuade the government, over time, to ban lead-based gasoline and paint across the country.
The work in El Paso was so thrilling that Landrigan abandoned his plans to return to life as a pediatrician. “In clinical pediatrics, you’re taking care of children one at a time,” he told me. “In public health, you’re taking care of whole communities.” From that point on, he decided, he would dedicate himself to public health. He worked for a couple of years on vaccination initiatives in Nigeria and El Salvador; founded what would eventually become the CDC’s National Center for Environmental Health; earned a couple of public health degrees from the University of London; and, in 1979, became the director of the field headquarters of the CDC’s National Institute for Occupational Safety and Health. Through it all, Landrigan kept up the hunt for environmental pollutants such as lead, asbestos, and arsenic. Another of his targets was a particularly nasty solvent called benzene, which had been the subject of a decade of court battles between the government and the chemical industry, and which finally came under regulation in the late eighties after a series of detailed investigations by Landrigan and his team.
Landrigan’s reputation grew with each new study, each new regulation that his work seemed to produce. And he was only getting started. In 1985, he became the director of the Environmental and Occupational Medicine division at the renowned Icahn School of Medicine at Mount Sinai, in New York. While he was there, the National Academy of Sciences formed a research committee to study the health effects of pesticides on children. Landrigan chaired the committee, which released a report in 1993 with the findings that children are far more sensitive than adults are to pesticides, and that, especially disturbing, kids are disproportionately exposed to such chemicals through their diet. The fallout from the report was extraordinary: It led to the 1996 Food Quality Protection Act, the creation of the EPA’s Office of Children’s Health Protection, and an executive order from President Bill Clinton that federal agencies had to consider children’s health when making policies.
The aggressiveness of Landrigan’s research and the urgency of his actions are belied by his calm and gentlemanly demeanor. He’s given more to fact-driven presentations than fist-pounding sermons. His passion “doesn’t always come out in fiery speech, in fact, it very seldom does,” said Gina McCarthy of the Harvard T.H. Chan School of Public Health. “But he has a fire in his belly.”
Landrigan told me that when it comes to children being exposed to dangerous pollutants, anger can be a prime motivator for his work. But “standing up and screaming doesn’t accomplish anything,” he said. “Instead, I use the anger as a source of energy and try to produce the data that are going to change things.” It’s an approach, he told me, that he picked up from his mentor, the pioneering occupational health researcher Irving Selikoff: “He used to say that statistics are people with the tears wiped off.”
* * *

Landrigan photographed at a meeting in 1975, during his tenure as an officer in the Epidemic Intelligence Service of the Centers for Disease Control. (Photo: Image courtesy CDC)
At 3 o'clock one afternoon this past April, Landrigan stood in front of thirty or so students enrolled in Case Studies in Epidemiology. The course, co-taught with Tom Chiles, was the first new class of the Global Public Health and the Common Good Program, which expands a popular public health concentration that already existed at Boston College. The public health program is separate from the Global Observatory on Pollution and Health, the other new initiative that Landrigan oversees at the University, but as you might expect, there’s some overlap. They are both components of Boston College’s new Schiller Institute for Integrated Science and Society, and in a sense, they function as the two branches of a new entity with the sweeping goal of improving health across the world. The public health program is the academic branch, while the observatory is primarily concerned with policy and research.
Though in existence for just a year or so, the observatory has plenty of projects already under way. There’s a collaboration with the UN to analyze just how much the pronounced air pollution in India costs that country in health care expenses and lost productivity, plus various other investigations into how pollution affects everything from children’s health to cardiovascular disease to cognitive and neurodegenerative disorders such as ADHD and dementia. Then there’s the work with the Prince Albert II of Monaco Foundation, which dates back to December, when Landrigan first met with the prince, His Serene Highness, and pitched the idea of studying a range of critical health threats in the ocean, including plastics, mercury, bacterial contaminants, and toxic algal blooms. In addition to these projects, the observatory is collaborating with the likes of the World Health Organization and Gina McCarthy’s Harvard Center for Climate, Health and the Global Environment, which plans to use research from the observatory to document how pollution also contributes to climate change.

Representing Boston College at the signing of a 2018 memorandum of understanding with the UN Environment Programme were Landrigan, right, and Vice Provost for Research and Deluca Professor of Biology Tom Chiles, second from left. The agreement was signed in advance of a BC Global Observatory on Pollution and Health study of pollution in India. (Photo: courtesy UN Environment Programme)
It was time for the class to begin, and as Landrigan prepared to address the students, Tom Chiles settled into a seat in the back of the room. On a projection screen behind Landrigan was a photo of an enormous plume of dust pouring from the collapsing Twin Towers on 9/11. When the towers came down, Landrigan told his students, they sent that toxic cloud of chemicals rolling through the streets of New York. At the time of the attacks, Landrigan was working at the nearby Mount Sinai. He and his colleagues coordinated a health-monitoring network for workers and first responders, and within weeks began seeing patients whose lungs had been seared with caustic cement dust and shredded with glass fibers and asbestos. “We were pulling gravel out of people’s lungs,” Landrigan told the class.
Nearly 20 years out, Landrigan said, any long-term health effects related to 9/11, such as cancers, would probably just now be showing up. At that point, hands in the room went up. How, his students asked, could people know whether any cancers were definitely related to 9/11? And what about the health of any children in utero when the attacks happened? The students were thinking like epidemiologists.
* * *
That, of course, is one of the primary goals of the public health program. In drawing on his own experiences, Landrigan wants to help train a new generation of public health professionals committed to saving lives and to helping the disenfranchised and vulnerable populations that are invariably the hardest hit by whatever poisons are introduced into the air, water, and soil.
As part of that process, Landrigan, Chiles, and leaders from Boston College’s Mission and Ministry led a small group of students on a weeklong service mission to Honduras last summer, showing them what health and health care look like in a poor, developing country. The group’s first visits were to wealthy, private clinics—clean, well-run facilities that wouldn’t have looked out of place in the States. Then they visited government-run centers, such as Hospital Santa Teresa. The patients there tended to come from extreme poverty, yet they had to provide their own bed sheets and pay for their own medicine and IVs. The private and public facilities “were so drastically different,” recalled Gabriella Taghian ’19, one of two student leaders on the trip. “It was the polar opposite. I was shaken by it.”

Landrigan, left, watched as Senator Richard Blumenthal of Connecticut spoke during a 2017 Washington, D.C., rally in support of a bill—so far unsuccessful—that would ban the pesticide chlorpyrifos. (Photo: Courtesy of the Office of Senator Richard Blumenthal)
Elsewhere on the trip, students discovered how poor the air quality can be in a developing nation, especially indoors, where many families still use traditional fires for cooking. Then there was the water. “We were driving in the van and we noticed this canal,” said Emily Zona ’19, the other student leader on the trip. “People were drinking from it, bathing, doing their laundry, and using it for a restroom.”
“It definitely touched us,” Taghian told me. Having just graduated, both she and Zona are planning to go into medicine, but, because of the trip, they are now looking for opportunities to work in public health before starting medical school. “Every decision that we’re making about our future,” Taghian said, “we always go back to Honduras and what we learned and how we felt there.”
Whatever the future holds for Taghian and Zona, Landrigan is confident that “the students we train at BC are going to go on and be leaders in this field. The enthusiasm that I’ve seen among the students for learning about these issues, for pursuing careers in these areas, is palpable. It’s a long-term investment. It’s going to take a few years to get them there, but I think the payoff is going to be enormous.”
* * *

Landrigan being interviewed by Anderson Cooper for a "60 Minutes" story about toxic formaldehyde emissions related to the laminate flooring found in many American homes. (Photo: courtesy CBS News)
The Global Public Health and the Common Good Program is currently an interdisciplinary six-course minor, built around a core of basic epidemiology and public health, with additional courses in law, ethics, economics, and social justice. By 2021, the university intends to expand it to a full twelve-course major. There are plans in the works to ramp up hiring as the program grows. “One of the goals is to recruit the next generation of faculty who can carry on when I am no longer here,” Landrigan told me.
When you’ve spent your career doing what Landrigan has, it can become second nature to see nothing but the world’s problems. But Landrigan said that, for all of our challenges, there are reasons for hope. After all, the levels of the six most common air pollutants in the U.S. have dropped by 70 percent thanks to the Clean Air Act. And in the decade after we began phasing lead out of gasoline, the average amount of lead found in our blood dropped by more than 90 percent—and, as a result, the collective IQ of the nation’s children rose by as much as five points.
Those successes, Landrigan said, required developing solutions to big problems. And if it worked for those big problems, he said, “there is no reason the basic strategies cannot be adapted” to solve the next ones we face.
Not long after I visited with Landrigan, he emailed me a photo from his trip to Monaco. It showed him among a group of government and science officials from the country. Near him stood the prince. In replying, I asked Landrigan whether he’d ever dreamt, way back during those early days in El Paso, that his career would eventually have him leading multinational research collaborations…and rubbing elbows with royalty. He wrote back with just two words: “Quite astounding.”
Shannon Fischer is a science writer who lives in Boston.
Share your thoughts: bcm@bc.edu