Sandra Leyan Castillo is a nurse practitioner in an orthopedic medical group—but with an important distinction: What sets this Boston College graduate apart from others in her field is that she is working in Chile as that country’s first-ever nurse practitioner.
While Leyan is a trailblazer, her path is likely to be followed by many others, thanks to a partnership between the BC Connell School of Nursing and Pontificia Universidad Católica de Chile (PUC), who together are educating Chile’s first nurse practitioners.
There is a pressing need for NPs in Chile, where access to care—particularly for those in rural areas and those cared for in the public hospitals—can be extremely difficult, according to Connell School Associate Dean for Graduate Programs Susan Kelly-Weeder, who is leading the effort to make nurse practitioners a reality in Chile.
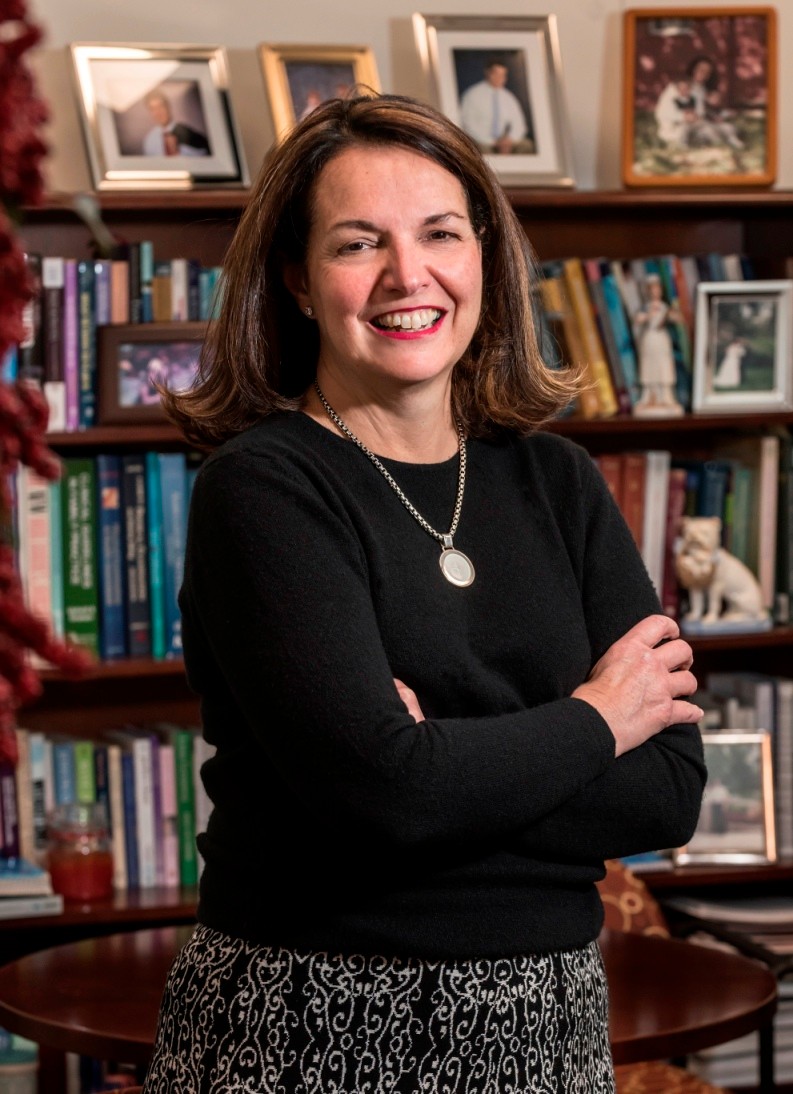
Connell School Associate Dean for Graduate Programs Susan Kelly-Weeder is leading the effort to make nurse practitioners a reality in Chile. (Lee Pellegrini)
Kelly-Weeder said patients cared for within the public health care system are required to seek help in specific community clinics that are often understaffed. Patients typically queue up hours before the clinics open and may have to return again the next day if health care providers are not able to see them.
“It’s a perfect time to introduce the NP role into both the public and private health care sectors,” explained Kelly-Weeder, a family nurse practitioner and associate professor in the Connell Shcool. “The first NPs in the U.S. were prepared to take care of individuals who were not able to access care. Loretta Ford was a public health nurse who saw that young children were not getting the care they needed. They were not being immunized or getting preventative care. In response, she developed, along with pediatrician Dr. Henry Silver, the first NP program, training registered nurses to provide primary care to pediatric patients.
“Today, the majority of NPs in the U.S. are educated as primary care providers and are managing care for individuals with acute and chronic illnesses across the lifespan.”
Currently in Chile, nurses earn a bachelor’s degree in nursing (a five-year program) but while graduate programs are available, none of them involve post-baccalaureate advanced practice nursing.
Last month, Kelly-Weeder made her fifth visit to Chile, where she taught an intensive session of her course The Role of the Advanced Practice Nurse to Chilean nurses who work in a variety of health care settings. She will teach the remainder of this course online for the 17 students. Since 2018, Kelly-Weeder has taught the course three times to approximately 75 students.
Leyan attended Kelly-Weeder’s class two years ago and expressed interest in furthering her education and becoming a nurse practitioner. With financial support from PUC, its hospital, and the Connell School, Leyan enrolled in the Connell School and earned a master’s degree in 2019. She passed a national certification exam and returned to Chile as a family nurse practitioner.
A second nurse from Chile who Kelly-Weeder also taught, Magdalena Correa Duque, is currently enrolled in the Connell School’s family nurse practitioner program and is expected to graduate in 2021.
"Interest in the role of the NP has increased dramatically in the five years I’ve been going to Chile. It’s a perfect time to introduce [nurse practitioners] into both the public and private health care sectors."
“I love being a nurse practitioner. It’s very exciting to talk to groups of nurses and physicians about what nurse practitioners can do,” said Kelly-Weeder, who is president-elect of the National Organization of Nurse Practitioner Faculties, an organization devoted to promoting high-quality nurse practitioner education.
The long-term goal is to establish a nurse practitioner master’s degree program at PUC, an objective supported by many physicians in Chile, said Kelly-Weeder, noting that limited access to care is a problem not only for those in rural areas or in the public health care system. She was told by a concerned oncologist that patients wait months to be seen—a critical and even deadly delay that doctors want to remedy.
Kelly-Weeder expects Chile’s nurse practitioner educational and practice model to replicate how NPs were first introduced in the U.S.: The nurses will be educated and certified as NPs for a particular population (pediatrics, adult, women’s health, psychiatric, or family); specializations, if desired, would follow the certification process and would require additional training and expertise.
A country lacking NPs also lacks NPs to serve as faculty members. So how will the nurses be educated? Kelly-Weeder says she expects to continue to teach in Chile, but that other faculty members at PUC could fill the role. For example, a pharmacist could teach Advanced Pharmacology and physicians could teach Advanced Health Assessment; physicians also can serve as preceptors for the short term. Eventually, Leyan, and other NPs who come after her, will take on these teaching roles.
Kelly-Weeder says PUC is a year or two away from having its NP program developed, approved, and ready for students.
As an indication of how committed Chile is about moving forward with the NP model, this spring representatives from the Chilean Ministry of Health plan to visit the Connell School and Boston hospitals and health care facilities to see firsthand nurse practitioners in the field.
“Interest in the role of the NP has increased dramatically in the five years I’ve been going to Chile,” said Kelly-Weeder. “I’ve come to love Chile. It’s a beautiful country with a warm and inviting population who are eager to see how nurse practitioners can improve the care in their country. I’m so delighted to be helping them in doing this work.”
Kathleen Sullivan | University Communications | February 2020