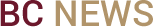University Health Services nurses Melissa DeNucci, R.N., and Yolanda Hobin, F.N.P., with medical record and technology assistant Margaret Bligh.
If there’s one department at Boston College that has the deepest, most up-close insight into the coronavirus pandemic, it’s University Health Services.
UHS had its eye on the virus well before COVID-19 began attracting media and public attention, increasing its vigilance and readiness as the outbreak began to proliferate. And UHS was at the forefront of the University’s battle against the disease when it came to campus.
Although an unprecedented event in many respects, the coronavirus crisis has shined a light on the special challenges of being a health care provider in a major university setting. For BC’s University Health Services personnel, the first months of 2020 tested not only their collective professional skills, but also their ability to adapt to fast-changing circumstances, collaborate with other BC offices and departments, and deliver different levels of care as necessary in an atmosphere of considerable anxiety about the threat of COVID-19.
The period of March 16, when UHS began testing for coronavirus, through April 22 offers a snapshot of the department’s activity. During this time, the department recorded 151 patient COVID-related contacts—by phone, telehealth sessions, or in-person visits—61 of which resulted in “unique” COVID-19 visits and evaluations. UHS administered 31 coronavirus tests on students living on or off campus; 17 of these were positive.
Such numbers barely hint at the day-in/week-out assortment of tasks and procedures that have made up the UHS effort against the coronavirus, even while continuing to meet students’ other health-related needs.
“I think Health Services has performed exceptionally well,” said UHS Director Thomas Nary, MD, in a recent interview. “We’ve gone by all the guidelines for health care workers as we’ve provided care to students who’ve needed it, and there have only been a few instances where someone had to miss a shift. Everybody showed up and did their jobs.”

Health and college life
A college campus is a unique place to be a health care professional, according to UHS staff: The community you serve is largely between the ages of 18 and 22, most of its members are unused to being responsible for their health care—many have never even gone to see a doctor on their own—and while generally very healthy, they don’t always make the best decisions on maintaining a healthy lifestyle. What’s more, the thousands in this community tend to live and socialize in close quarters, whether on or off campus, and at various times of the academic year may be in another part of the country, or the world.
But ask Caroline Faherty, a registered nurse who’s been at UHS for almost 14 years, how she likes the job, and she is happy to tell you.
“I love working with the students,” she said. “You get to see many of them over the course of four years, and you can definitely create a bond with them. It’s great to see them learning how to take care of and advocate for themselves, how to use resources, and manage their care.”
Theresa Barba, a 30-year veteran of BC Health Services—whose mother was the nurse manager when the facility was on Newton Campus—agrees with her fellow registered nurse.
“This age group has a lot to offer,” she said. “They’re all very bright, very eager to make their own way, and we try to give them the tools to lead healthy lives, whether through our health education programs or if they should happen to visit our primary care center.”

Associate Director for Health Services Operations Scott Jusseaume, M.D.
UHS Associate Director Scott Jusseaume, M.D., points to the approximately 21,000 visits a year by students to the UHS ground-level facilities at the Thomas More Apartments on Lower Campus as a measure of the department’s role at BC.
“We are it. We are the health care provider on campus,” he said, noting the UHS response to a norovirus in late 2015 that sickened 140 BC students. “We deal with illnesses, injuries, chronic health issues—we are a full-bore medical practice.”
To fulfill its responsibilities as a health care provider, UHS has to be cognizant of what happens elsewhere in Massachusetts, the U.S., and the world, even as it tends to the health and well-being of BC students. As a matter of course, Jusseaume stays in touch with the Massachusetts Department of Public Health and the Centers for Disease Control on, for example, flu outbreaks and other potential public health risks.
Some UHS staff work in other health care settings, and know other health care professionals—other potentially useful sources for getting a read on emerging health threats. Then there are the warning signs “on the ground,” according to UHS staffers: an increase in calls from students concerned about their health or that of a roommate or friend, or from BC parents worried that their child might be ill.
Caroline Faherty, R.N., and University Health Services Director Thomas Nary, M.D.
UHS staffers knew that during the semester break some BC students had traveled to China and South Korea, identified as coronavirus hot spots, or parts of Europe starting to emerge as affected areas, and began urging those exhibiting symptoms or concerned that they might be infected to contact the department or their health care providers. UHS worked with other departments to increase health safeguarding measures—already in effect for the flu season—for common areas and touchpoints on campus, and was part of the BC Emergency Management Team, which coordinated the University’s response to the coronavirus and kept the campus community informed of news and updates concerning the pandemic.
Later, when all but several hundred students left campus following the suspension of on-campus classes, UHS worked with Residential Life and the Emergency Management Team to set up the Thomas More Apartments residence hall as an area to quarantine students awaiting COVID-19 test results or isolate those testing positive.
“Our partnership with other offices and departments, like Dining Services, Facilities Services, Residential Life, BC Police, and so on, has always been important to protecting health on campus,” said Nary. “They have all done an amazing job, and have made it possible for us to do our job.”
Sisters-in law Jacqueline Mullowney, R.N., and Maureen Mullowney, R.N.
"You have to be on your game."
Throughout February and then into March, UHS experienced a rise in visits and calls from students complaining of illness, although not necessarily from the coronavirus, since the flu was still an ongoing concern. For their own safety, as well as those of students seeking care, the UHS staff had to keep up to date on recommendations from the CDC and other authorities on how health care sites should be organized and what practices medical worker should follow: UHS staff were given a list of specific questions to ask in response to phone calls, e-mails, or other contact from students; students showing signs of coronavirus had to be directed to a separate entrance to the UHS facility; chairs had to be cleared out of the facility’s waiting room; all staff had to wear personal protective equipment.
“Every day was like a school day for us,” said Faherty. “We learned not only about dealing with the coronavirus, but about ourselves and how we treat people.”
When you are caring for sick people, especially those who may have an infectious disease that has been making headlines over the world, there is a certain way you have to be, according to UHS staff. You show concern and empathy, but to a certain degree you also have to be businesslike.
“You have to be on your game, be ready to offer explanations,” said Barba. “You know they’re worried about what’s going on, whether they might be in danger. But you have to get them to listen to you, because you have to educate them. You say, ‘This is what you have to look for. This is what you have to do. This is who you call.’ And you have to get them to think beyond themselves: ‘Don’t be in contact with other people, because you might make them sick.’”
“Having staff show that confidence helps when students come in,” said Jusseaume. “They’ve had to do so much, learning and assimilating new protocols in an environment that’s more dangerous than usual. They’re showing up to work, at some risk to themselves, and they’re providing good care.”
According to Nary and Jusseaume, UHS has received health-related updates from most of the students returning to the U.S.—and going directly home instead of to BC—from coronavirus-affected areas abroad, as well as others who left campus after on-campus classes were suspended. This has been helpful in tracking the progress of the disease in the BC community, they said.
“It is really is about cura personalis—care of the individual,” said Nary. “That’s a big part of what we teach at BC, and in a case like this, we want people to care not just for themselves but for others. I think that the students have done very well in that regard.”

Clockwise from left: Adminstrative Assistant Yvette Johnson; Associate Director Scott Jusseaume, M.D.; Director Thomas Nary, M.D.; Health Services Aide Anna Tom; Medical Record and Technology Assisant Margaret Bligh; Theresa Barba, R.N.; Maureen Mullowney, R.N.; Caroline Faherty, R.N.
Looking, and planning, ahead
As April came to an end, UHS continued to monitor the health of the 267 students remaining on campus, and the approximately 500-600 still living off-campus. The end of the academic year—one unlike any other in memory—was in sight, and the department was already starting to think about the next, despite the uncertainty throughout higher education as to what format should be adopted for the 2020-21 academic year.
“It’s always part of our routine to debrief and look back,” said Jusseaume. “This time, obviously, we’ll have a lot more to review: Did we communicate effectively? Were there changes we should’ve implemented sooner? That’s where we’ll be in a few weeks.”
In addition to keeping track of the pandemic, and helping the University devise its operating plans for the coming academic year, Nary noted that he and his colleagues will spend the summer updating health records for returning students, and familiarizing themselves with the new group of students who will be coming to campus.
“Certainly, we’ll be thinking a lot about the coronavirus, but as always, we’re concerned with all the health needs of our students, especially those who have chronic or underlying conditions,” he said. “So over the summer, we’ll reach out and introduce ourselves, make sure everyone knows who and where we are. It’s very important to have that rapport, because if and when the time comes when they need health care—whether it’s coronavirus or anything else—you want them to know whom they can turn to.”
Sean Smith | University Communications | May 2020